Figures at the front line of the opioid fight

Editor’s note: This is the third of a five-part series by West Hawaii Today focusing on opioid addiction on Hawaii Island. Itbegins with how a heroin overdose played a vital role in the shuttering of a well-known Kailua-Kona homeless camp andfinishes on what more needs to be done to fight painkiller abuse. Eye-opening stats will be presented along the way: HawaiiCounty’s prescription rate doubles every other county in the state, while a vast majority of overdose calls are in homes andcondos, not in homeless sites.
Editor’s note: This is the third of a five-part series by West Hawaii Today focusing on opioid addiction on Hawaii Island. Itbegins with how a heroin overdose played a vital role in the shuttering of a well-known Kailua-Kona homeless camp andfinishes on what more needs to be done to fight painkiller abuse. Eye-opening stats will be presented along the way: HawaiiCounty’s prescription rate doubles every other county in the state, while a vast majority of overdose calls are in homes andcondos, not in homeless sites.
Day 2: Averted or inevitable? Hawaii numbers lower than mainland, but officials wary
Day 3: Figures on the front: Meeting the faces and agencies fighting against opioid abuse
Day 4: Lessons learned: Safeguards, prevention improved with knowledge gained
Day 5: Coming out the other side: More is needed in the fight, but recovery story proof it works
^
KAILUA-KONA — In an office tucked back behind a Taco Bell, around the corner and through a door marked with a large red ribbon works a team of professionals on the frontlines in a fight for people’s lives.
It’s a formidable task. But the team from the Hawaii Island HIV/AIDS Foundation and the Hawaii Health and Harm Reduction Center are up to it, undaunted even.
“The population that we serve, the few minutes that they’re in here with us is probably the calmest and the safest moments of their day, just because of the whole attitude of the staff,” said Bud Luth, community health outreach worker with HIHAF and the Hawaii Health and Harm Reduction Center. “We’ve got people that’ll come by to exchange and they just want to hang out, because it’s a safe place to be.”
While addiction recovery resources in West Hawaii are limited, particularly when it comes to residential treatment centers — considered the “gold standard” of treatment, as one expert put it — health professionals throughout the region are working to help residents change their lives.
HIHAF, through its collaboration with the Hawaii Health and Harm Reduction Center, is one of them, exchanging anywhere from 10,000 to 15,000 needles a month in its Palani Road office as part of a statewide syringe exchange program overseen by the Hawaii Health and Harm Reduction Center.
It runs on a specific model geared toward harm reduction, where the approach is to center the health and well-being of clients, such as those whose use of injection drugs puts them at high risk of contracting HIV as well as Hepatitis-B and -C in addition to risk of an overdose, without passing judgment on the client.
“It means we meet people where they’re at,” said Teri Hollowell, director of programs at HIHAF. “We don’t preach. It’s not about abstinence.”
The great thing about it, she said, is it “brings the trust in,” drawing in people who might otherwise be apprehensive about coming through HIHAF’s doors.
And clients do, in their own time, start to engage with staff, which would give the staff an opportunity to make referrals — if, Hollowell noted, there were any place to refer them.
Through the syringe exchange program, Luth and Hollowell say the harm reduction approach also provides an opportunity to educate their clients about resources that could literally save their lives.
DRUGS TO COMBAT DRUGS
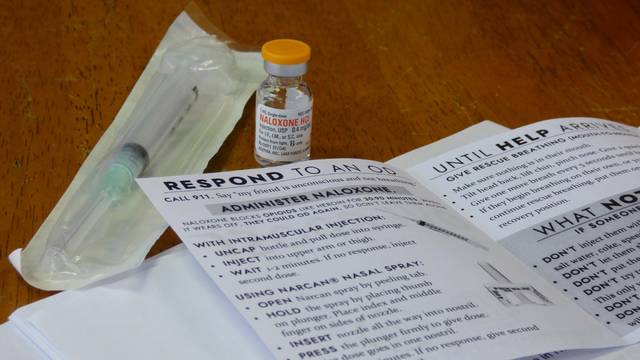
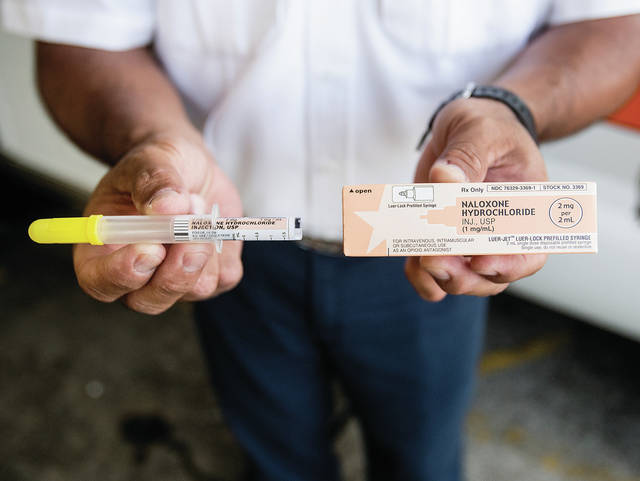
If a client in the syringe exchange program indicates they are using opiates, for example, Luth said he’ll introduce them to naloxone, a drug that blocks opioid receptors and reverses an overdose’s toxic effects, according to the federal Substance Abuse and Mental Health Services Administration. Naloxone can be injected via a syringe and is also available as a nasal spray.
An option for those being treated for opiod use disorder includes buprenorphine, which can mitigate symptoms of withdrawal, which while not life-threatening, can be severe.
Buprenorphine is what’s considered a “partial agonist” and, similar to full agonists like heroin and hydrocodone, can produce a feeling of euphoria. Unlike full agonists though, in which the effects continue to increase with the dose, the effects associated with buprenorphine eventually hit a ceiling and level off, reducing the risk of misuse or dependency.
Both Dr. Michael McGrath of the Recovery Enhanced Medicine Institute (REMI) and Dr. Laura Ankrum, a family practice doctor at West Hawaii Community Health Center, are able to prescribe buprenorphine, as is Dr. Stephen Denzer, medical director at Hawaii Island Recovery.
ASKING THE RIGHT QUESTIONS
But treatment and recovery isn’t just about replacing one kind of drug with a buprenorphine prescription, and REMI, Hawaii Island Recovery and the West Hawaii Community Health Center all use multi-pronged approaches that extend well beyond medication.
Given West Hawaii Community Health Center’s position as a community clinic, that approach starts right at the door.
The clinic serves about a quarter of the West Hawaii population, a range that runs from Kawaihae to Ocean View — 80-plus miles the way the crow flies. In 2016, 72 percent of their patients were receiving Medicare or Medicaid and a little over 56 percent were at or below the poverty line, according to federal data.
The clinic has adopted several measures to cast as wide a net as possible to help people who might have an undiagnosed use disorder.
Among those steps is a universal screening, with a goal of asking 100 percent of adults about substance use — tobacco, alcohol and other drugs — at least once a year, said Dr. Diane Logan, clinical psychologist and substance use coordinator at West Hawaii Community Health Center.
Asking those questions is critical because a person might have a substance use disorder, but it’s not what’s bringing them through the clinic’s doors.
“They come in because they fell last night and they have a bruise,” Logan said. “And we happen to ask the right question.”
And if they didn’t ask, they wouldn’t know, which is why they’ve moved in the last couple years toward asking everybody about substance use.
“Because we don’t want to miss those opportunities,” Logan said.
The clinic’s approach also includes brief interventions for those with mild or moderate use disorders and don’t necessarily need months-long residential or out-patient treatment.
Instead, Logan said, the brief intervention focuses on “working with patients where they are” to increase their motivation to change behaviors and explore what steps people can make or identify how the clinic can help.
From 2015-17, West Hawaii Community Health Center saw increases in visits and patients where opioid use disorder was billed, from 81 patients with 207 visits in 2015 to 146 patients with 1,267 visits in 2017.
There’s an important caveat there, though: That rise doesn’t necessarily mean an increase in use.
“It means that we’re doing a better job of asking,” Logan said, referencing screening protocols the clinic has established. “We’re doing a better job of asking earlier on and there’s good word of mouth about our program and clinic where people are not afraid to come in and ask.”
TREATING OUTSIDE THE BOX
Doctors are also recognizing the value of incorporating alternatives to and alongside medication, which includes an emphasis on exercise or diet as a prescription, rather than just pharmaceuticals.
“We know that active treatment works better,” Logan said. “Exercise, physical therapy, behavioral health — things where people are doing things versus taking things, for long-term benefit.”
The Recovery Enhanced Medicine Institute’s facilities include a dojo, massage and “mind elements” like mindfulness therapies and group therapies, while Hawaii Island Recovery’s services covers not only medically supervised detox and residential care but also incorporates an approach that evaluates each person’s unique needs and situation to establish a treatment plan, incorporating everything from neurofeedback, which works directly with the brain to regulate itself, to holistic approaches like acupuncture and yoga.
McGrath noted that an important consideration is for chronic pain patients, who would otherwise suffer without some sort of strong pain relievers.
In those cases, he said, it’s important to find “the most risk-reduced” option, which can include anti-epileptics and anti-depressants that have pain relieving properties as well as topicals like capsaicin, the substance that gives chili peppers their heat.
WRAPAROUND HEALING COVERS ALL ASPECTS OF HEALTH
A treatment plan also must get to the heart of identifying a client’s trauma and set them up to succeed when they ultimately leave treatment.
The addiction medicine program at West Hawaii Community Health Center comes with a slate of wraparound resources.
It starts with an intake evaluation to learn about the patient’s history and identify their unique needs, using a team approach that involves a series of appointments before a patient even sees a prescriber about buprenorphine.
Once a patient’s needs are identified, said Alysa Lavoie, case manager at the West Hawaii Community Health Center, a treatment plan is developed to determine which providers ought to be included. There’s always a prescriber, as well as a clinical psychologist or licensed clinical social worker and a case manager to organize wraparound services like housing referrals, family services, help with obtaining insurance and public assistance as well as making referrals to higher levels of care, if needed.
“As the physician in the program, it’s really important to have our team together, and we rely on each other,” said Ankrum. “And that’s been a big factor why I think our program has been successful.”
But what’s also important is the situation clients are able to get into once they leave treatment and identify ways they can continue their recovery.
One factor Hawaii Island Recovery admission director Jimmy Kayihura identified for finding success post-treatment is finding and developing structure. That structure is what residential treatment provides, and replicating that after leaving treatment — through meetings, exercise, consistent sleep schedules and more — goes a long way in getting back “into the stream of life.”
Eliza Wille, program director and therapist at Hawaii Island Recovery, said clients are tracked for a year after completing treatment and check in at certain times throughout the year.
The percentage of clients who report being sober a year after finishing treatment has been somewhere in the 70s the last couple years, she said.
“That is definitely much higher than the industry average,” she said. “And we’re really proud of that.”
RECOVERY A JOURNEY, NOT A DESTINATION
While abstinence is the ideal for opioid use disorder and drug-free treatment the ideal for chronic pain, McGrath said the work toward that goal is “a journey, not a destination,” pointing to what he said can be a double standard with addiction.
Treatment programs, he said, sometimes require patients to be entirely abstinent, sometimes giving patients an ultimatum of one year on buprenorphine before withdrawing assistance entirely.
He drew a line to Type II diabetes, where the goal is to manage it with diet and exercise, though most patients will be prescribed medications.
“Would we give people one year of insulin or one year of their metformin for their diabetes and say, ‘You didn’t diet and exercise, you still weigh 350 pounds, you know what, we’re cutting you off?’” he said. “Absurd, right? But that’s what we do with addiction.”
Ankrum made a similar point about the traditional approach that cuts people off.
“Any other chronic health condition, if the patient’s getting worse, we increase treatment,” she said. “Traditionally with substance use, if the patient gets worse, we cut them off, which doesn’t make sense, right? If somebody’s numbers are going up, we’re going to do more to treat them.”
^
RESOURCES FOR HELP
If you or someone you know may have a substance use disorder, including opioid use disorder, the following is a list of agencies and other resources referenced in this series:
Hawaii Island HIV/AIDS Foundation
* Phone: (808) 331-8177
* Web: www.hihaf.org
Hawaii Island Recovery
* Phone: (877) 721-3556
* Web: www.hawaiianrecovery.com
Recovery Enhanced Medicine Institute (REMI)
* Phone: (808) 498-4102
* Web: www.recoveryenhancedmedicine.com
West Hawaii Community Health Center
* Phone: (808) 326-5629 (For emergencies, always call 911)
* Web: www.westhawaiichc.org
Hawaii Department of Health Alcohol and Drug Abuse Division (Hawaii Island)
The following Hawaii Island agencies are included in a list of agencies funded by ADAD.
^ Big Island Substance Abuse Council
*West Hawaii – (808) 322-3100 / East Hawaii – (808) 935-4927 / North Hawaii – (808) 887-2175
^ Bridge House, Inc. (Kona)
* Phone – (808) 322-3305
^ Ku Aloha Ola Mau (Formally DASH) (Hilo)
* Hilo – (808) 961-6822
^ The full list of agencies funded by ADAD throughout the state is available at health.hawaii.gov/substance-abuse/prevention-treatment/treatment/treatment-services
Substance Abuse and Mental Health Services Administration
The hotline is a confidential, free 24-hour/365-day-a-year service in English and Spanish
* Phone – 1-800-662-HELP (4357)